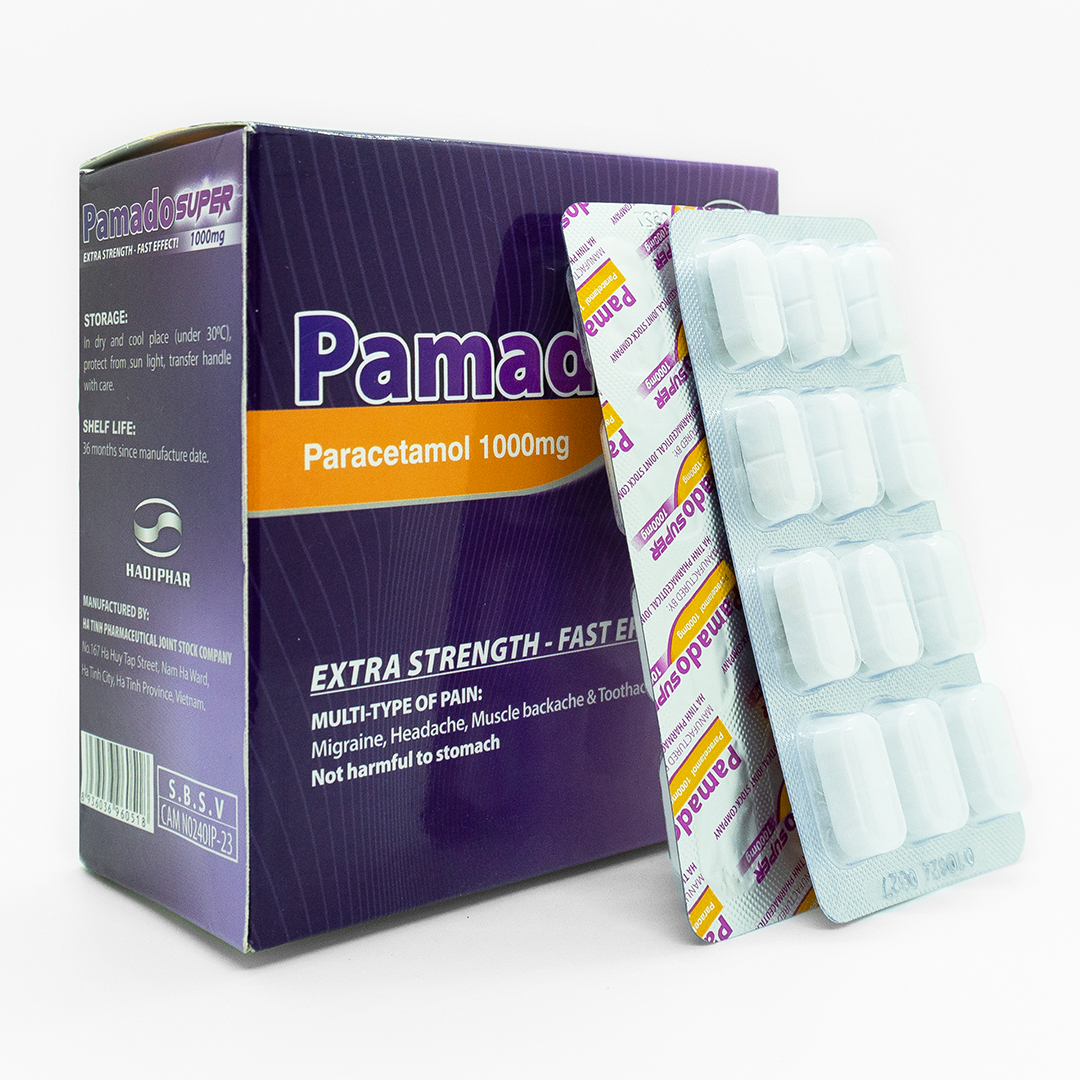
Designation:
Paracetamol is widely used in the treatment of mild to moderate pain and fever.
Pain
Paracetamol is used to temporarily relieve pain in the treatment of mild to moderate pain. The most effective medication is to relieve low-intensity pain of non-visceral origin. Paracetamol has no effect on rheumatic treatment. Paracetamol is an alternative to salicylates (preferred in patients with contraindications or intolerance to salicylates) for mild pain or fever.
Fever
Paracetamol is often used to lower body temperature in febrile patients, when fever can be harmful or when fever is reduced, the patient will be more comfortable. However, antipyretic therapy is generally nonspecific, does not affect the course of the underlying disease, and may mask the patient’s condition
Usage and Dosage
Dosage:
– Adults: The usual oral dose is 0.5g-1g/time (1 caplet), every 4-6 hours, up to a maximum of 4g/day.
– Children:
*Pain, fever:
+ From 6-8 years old: 240-250 mg;
+ From 8-10 years old: 360-375 mg
+ From 10-12 years old: 480-500 mg;
+ From 12-16 years old: 480-750 mg;
+ From 16-18 years old: 500 mg-1g;
Can repeated after 4-6 hours if necessary, up to a maximum of 4 doses/24 hours..
*Pain after surgery:
+ From 6-12 years old: 20-30 mg/kg (maximum 1g), a single dose, then 15-20 mg/kg, every 4-6 hours, up to 75 mg/kg/24 hours (maximum 4g/24 hours), divided into several small doses.
+ From 12-18 years old: 1g every 4-6 hours (maximum 4 doses/24 hours).
Note: For malnourished children, low weight, use dose 10mg/kg/hb5x
Hepatic impairment: Use with caution, use low doses. Avoid prolonged use.
Usage:
Paracetamol is usually taken orally.
Paracetamol should not be used for self-administration of pain for more than 10 days in adults or more than 5 days in children unless directed by a physician, as such severe and persistent pain may be a sign of a medical condition. It requires a physician to diagnose and treat with close supervision. Do not give paracetamol to adults and children for self-treatment of high fever (above 390C), fever lasting more than 3 days, or recurrent fever, unless directed by a physician, as such fever may be a sign Signs of a serious illness requires prompt diagnosis by a physician. To minimize the risk of overdose, children should not be given more than 5 doses of paracetamol to relieve pain or reduce fever in 24 hours, unless directed by a physican.
Contraindications
– Patients with anemia repeatedly or have heart, lung, kidney or liver disease.
– Patients with hypersensitivity to paracetamol.
– Patients with glucose-6-phosphate dehydrogenase deficiency.
Warnings and Cautions When Taking Drugs
Serious skin side effects, although the incidence is not high, but serious, even life-threatening, include Steven-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN) and toxic epidermal necrolysis (TEN).) or Lyell’s syndrome, acute generalized exanthematous pustulosis (AGEP).
Symptoms of the above syndromes are described as follows:
– Steven-Johnson syndrome (SJS): is a bullous drug allergy, blisters localized around the natural cavities: eyes, nose, mouth, ears, genitals and anus.
In addition, there may be high fever, pneumonia, liver and kidney dysfunction. Steven-Johnson syndrome (SJS) is diagnosed when at least 2 natural niches are involved.
– Toxic necrosis syndrome (TEN): is the most severe form of drug allergy, including:
+ Various skin lesions: measles-like rash, scarlet fever rash, erythema or blistering blisters, lesions quickly spread throughout the body;
+ Injury to the eye mucosa: keratitis, purulent conjunctivitis, corneal ulcer.
+ Injury to gastrointestinal mucosa: stomatitis, oral mucosal erosion, pharyngitis, pharynx, esophagus, stomach, intestine.
Damage to the mucous membranes of the genital tract and urinary tract.
+ There are also severe systemic symptoms such as fever, gastrointestinal bleeding, pneumonia, glomerulonephritis, hepatitis… high mortality rate of 15-30%.
– Acute generalized exanthematous pustulosis (AGEP): small sterile pustules arising on a background of widespread erythema. Lesions usually appear in folds such as armpits, groin and face, then can spread to the whole body. The common systemic symptoms are fever, elevated neutrophil blood test.
At the first sign of skin rash or any other sign of hypersensitivity reaction, the patient should stop using the drug. People who have experienced serious skin reactions caused by paracetamol should not take the medicine again and when they come for medical examination and treatment, they need to inform the medical staff about this problem.
Paracetamol should be used with caution in people with liver failure, kidney failure, alcoholics, chronic malnutrition or dehydration.
Paracetamol must be used with caution in patients with pre-existing anemia because cyanosis may not be evident, despite dangerously high concentrations of methemoglobin in the blood.
Excessive alcohol consumption can increase the hepatotoxicity of paracetamol, so avoid or limit alcohol consumption
Use of Drugs for Pregnant and Breastfeeding Women
Pregnant:
The safety of paracetamol used during pregnancy has not been established in relation to possible adverse effects on fetal development. Therefore, paracetamol should be used in pregnancy only when clearly needed.
Breastfeeding women: In a study in mothers taking paracetamol after lactation, no adverse effects were found in breastfed infants.
Effects of the Drug on the Ability to Drive and Use Machines
The drug does not affect the ability to drive and use machines.
Drug Interactions and Incompatibilities
Long-term intake of high doses of paracetamol slightly increases the anticoagulant effect of coumarin and indandion derivatives. This effect seems to be of little or no clinical importance, so paracetamol is preferred over salicylates when mild pain relief or fever reduction is required in patients taking coumarin or indandion derivatives. Attention should be paid to the potential for severe hypothermia in patients receiving concomitant phenothiazines and antipyretic therapy.
Excessive and long-term alcohol consumption can increase the risk that paracetamol will cause liver toxicity.
Anticonvulsants (including phenytoin, barbiturates, carbamazepine) induce enzymes in the liver microsomes, which may increase the hepatotoxicity of paracetamol by increasing the metabolism of the drug into substances that are toxic to the liver.
In addition, concomitant administration of isoniazid with paracetamol may also lead to an increased risk of hepatotoxicity, but the exact mechanism of this interaction has not been determined.
The risk of paracetamol causing hepatotoxicity is significantly increased in patients taking larger than recommended doses of paracetamol while taking anticonvulsants or isoniazid. No dose reduction is usually required in patients receiving concomitant therapeutic doses of paracetamol and anticonvulsants; However, patients must limit self-administration of paracetamol while taking anticonvulsants or isoniazid.
Probenecid may decrease the elimination of paracetamol and increase the half-life of paracetamol.
Isoniazid and anti-tuberculosis drugs increase the toxicity of paracetamol to the liver
Since there are no incompatibility studies, this drug should not be mixed with other drugs.
Undesirable Effects
Skin rashes and other allergic reactions occur occasionally. Usually erythema or urticaria, but sometimes more severe and may be accompanied by drug fever and mucosal lesions. Patients with hypersensitivity to salicylates are rarely sensitive to paracetamol and related drugs. In rare cases, paracetamol has caused neutropenia, thrombocytopenia and pancytopenia.
Uncommon, 1/1000 < ADR < 1/100
Sold.
Stomach-intestines: Nausea, vomiting.
Hematology: Hematopoietic disorders (neutropenia, pancytopenia, leukopenia), anemia.
Kidney: Kidney disease, nephrotoxicity with long-term abuse.
Rarely, ADR <1/1000
Other: Hypersensitivity reactions.
Instructions on how to handle ADR
If serious side effects occur, stop taking paracetamol. For treatment, please read the section: “Overdose and Management”..
Immediately notify your doctor or pharmacist of any adverse reactions encountered while using the drug.
Overdose and Treatment
Expression
Paracetamol toxicity can be caused by a single toxic dose, by repeated ingestion of large doses of paracetamol (eg, 7.5 to 10 g per day, for 1 to 2 days), or by long-term administration. Dose-dependent hepatic necrosis is the most serious acute toxic effect of overdose and can be fatal. Nausea, vomiting, and abdominal pain usually occur within 2 to 3 hours of taking a toxic dose of the drug. Methemoglobin – blood, leading to cyanosis of the skin, mucous membranes and nails is a characteristic sign of acute poisoning with p-aminophenol derivatives; A little of sulfhemoglobin may also be produced. Children tend to make methemoglobin more easily than adults after taking paracetamol. In severe poisoning, there may be initial CNS stimulation, agitation, and delirium. This may be followed by central nervous system depression; stupor, hypothermia; exhausted; rapid, shallow breathing; fast, weak, irregular pulse; low blood pressure; and circulatory failure. Vascular collapse due to relative hypoxia and because Shock can occur if multiple vasodilation. Fatal choking convulsions may occur. Usually coma occurs before sudden death or after several days of coma. Clinical signs of liver damage become apparent within 2 to 4 days after ingestion of a toxic dose. It is possible that 10% of patients with untreated poisoning have severe liver damage; of which 10% to 20% eventually die of liver failure. Acute renal failure also occurs in some patients. Liver biopsy revealed central lobular necrosis except for the periportal portal region. In non-fatal cases, liver damage is reversible after weeks or months.
To Solve:
Early diagnosis is important in the treatment of paracetamol overdose. There are methods for rapid determination of drug plasma concentrations. However, treatment must not be delayed pending test results if the history suggests a severe overdose. When intoxication is severe, it is important to provide active supportive treatment. Gastric lavage in all cases, preferably within 4 hours after ingestion. The main detoxification therapy is the administration of sulfhydryl compounds, perhaps acting in part by replenishing the hepatic stores of glutathione. N-acetylcysteine is effective when taken orally or intravenously. The medicine must be given immediately if it has not been 36 hours since paracetamol has been taken. Treatment with N-acetylcysteine is more effective when given for a long time less than 10 hours after taking paracetamol. When giving orally, dilute the N- acetylcysteine solution with water or a non-alcoholic beverage to obtain a 5% solution and must be drunk within 1 hour after mixing. Give oral N- acetylcysteine with the first dose of 140 mg/kg, then give another 17 doses, each dose of 70 mg/kg every 4 hours. Discontinue treatment if plasma paracetamol test shows low risk of hepatotoxicity. Adverse effects of N-acetylcysteine include skin rash (including urticaria, which does not require discontinuation), nausea, vomiting, diarrhea, and anaphylactoid reactions. If N-acetylcysteine is not available, methionine can be used (see monograph Methionine). In addition, activated charcoal and/or salt bleach can be used, which can reduce the absorption of paracetamol.
STORAGE:
In dry and cool place (under 30°C), protect from sunlight, transfer handle with care.
SHELF LIFE:
36 months since manufacture date.
MANUFACTURED BY:
HA TINH PHARMACEUTICAL JOINT STOCK COMPANY