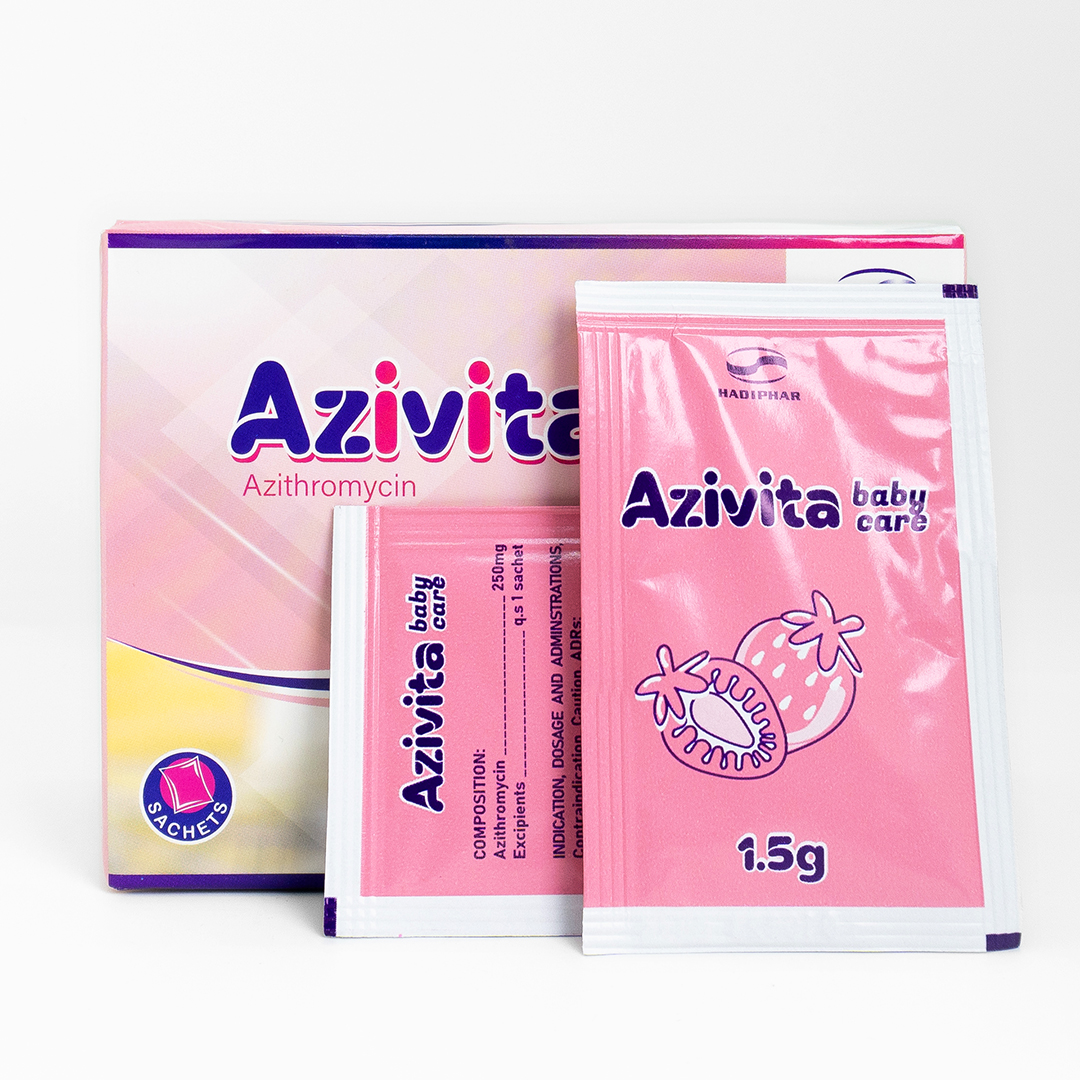
INDICATION:
- Treatment of infections caused by susceptible organisms.
- Treatment of lower respiratory tract and upper respiratory tract infections.
- Treatment of uncomplicated genital infections caused by Chlamydia trachomatis.
- Treatment of disseminated MAC infection (DMAC) in patients with advanced HIV infection.
INDICATION:
– Treatment of infections caused by susceptible organisms; in lower respiratory tract infections including bronchitis and pneumonia, in oral and dental infections, in skin and soft tissue infections, in acute otitis media and in upper respiratory tract infections including sinusitis and pharyngitis/tonsillitis.
– Treatment of uncomplicated genital infections due to Chlamydia trachomatis. It is also indicated in the treatment of chancroid due to Haemophilus ducreyi and uncomplicated genital infections due to non-multiresistant Neisseria gonorrhoeae.
Prophylaxis against Mycobacterium avium-intracellulare complex (MAC) infection or use in combination with ethambutol for the treatment of disseminated MAC (DMAC) infection in patients with advanced HIV infection.
USER TARGET:
– People who have respiratory problems such as bronchitis, pneumonia, sinusitis, tonsillitis, sore throat
– People encounter symptoms of soft skin and tissue infections,
– Uncomplicated genital tract infections caused by Chlamydia trachomatis or Neisseria gonorrhoeae are not multidrug resistant.
DOSAGE AND ADMINISTRATION:
Azithromycin is administered once daily, 1 hour before a meal or 2 hours after a meal.
Adults:
– Upper and lower respiratory tract infections, skin and soft tissue infections: 500mg in the first day; 4 days later: 250mg per day.
– Sexually transmitted diseases: a single dose of 1g.
Children:
– First day: 10mg/kg body weight/day. From day 2 to day 5: 5mg/kg body weight/day.
– Or as directed by a doctor.
CONTRAINDICATIONS:
Hypersensitivity to Azithromycin or to any of the ingredients.
WARNING AND IMPORTANT WHEN USING DRUGS:
Talk with your doctor or pharmacist before taking Azithromycin if:
You have severe liver or kidney problems.
You have severe heart problems or problems with your heart beat such as long QT syndrome (shown on an electro-cardiogram or ECG machine).
Your blood levels of potassium or magnesium are too low.
You develop signs of another infection.
You are taking any ergot derivatives such as ergotamine (to treat migraine) as these medicines should not be taken together with Azithromycin (see section “Taking other medicines”).
You have a certain type of muscle weakness called myasthenia gravis.
You have nervous (neurological) or mental (psychiatric) problems.
USING DRUGS FOR PREGNANT AND LACTATING WOMEN
PREGNANT:
– There are no adequate and well-controlled studies on the use of azithromycin in pregnant women. In reproduction toxicity studies in animals azithromycin was shown to pass the placenta, but no teratogenic effects were observed (see section 5.3). The safety of azithromycin has not been confirmed with regard to the use of the active substance during pregnancy. Therefore azithromycin should only be used during pregnancy if the benefit outweighs the risk.
BREASTFEEDING PERIOD:
– Azithromycin is excreted in breast milk. Because of the long half-life, accumulation in the milk is possible. Information available from published literature indicates that, in short-term use, this does not lead to clinically relevant quantities in the milk. No serious side effects have been observed by azithromycin in breast-fed children.
– A decision should be taken whether breastfeeding is discontinued or that treatment with azithromycin is discontinued/initiated or not, taking into account the benefit of breastfeeding for the child and the benefit of treatment for the woman.
UNDESIRABLE EFFECTS:
The table below lists the adverse reactions identified through clinical experience and post-marketing surveillance by system organ class and frequency. Adverse reactions identified from post-marketing experience are included in italics. The frequency grouping is defined using the following convention: Very common (≥ 1/10); common (≥ 1/100 to < 1/10); uncommon (≥ 1/1,000 to < 1/100); rare (≥ 1/10,000 to < 1/1,000); very rare (< 1/10,000); not known (cannot be estimated from the available data). Within each frequency grouping, undesirable effects are presented in order of decreasing seriousness.
OVERDOSE AND TREATMENT:
FOR AZITHROMYCIN:
Symptom:
The typical symptoms of an overdose with macrolide antibiotics include reversible loss of hearing, severe nausea, vomiting and diarrhoea.
To solve:
In the event of overdose the administration of medicinal charcoal and general symptomatic treatment and supportive measures are indicated as required
PHARMACOLOGICAL PROPERTIES:
PHARMACODYNAMICS:
Mode of action:
Azithromycin is an azalide, a sub-class of the macrolid antibiotics. By binding to the 50S-ribo- somal sub-unit, azithromycin avoids the translocation of peptide chains from one side of the ribosome to the other. As a consequence of this, RNA-dependent protein synthesis in sensitive organisms is prevented.
PK/PD relationship
For azithromycin the AUC/MIC is the major PK/PD parameter correlating best with the efficacy of azithromycin.
Following the assessment of studies conducted in children, the use of azithromycin is not recommended for the treatment of malaria, neither as monotherapy nor combined with chloroquine or artemisinin based drugs, as non-inferiority to anti-malarial drugs recommend- ed in the treatment of uncomplicated malaria was not established.
Mechanism of resistance:
Resistance to azithromycin may be inherent or acquired. There are three main mechanisms of resistance in bacteria: target site alteration, alteration in antibiotic transport and modification of the antibiotic.
Complete cross resistance exists among Streptococcus pneumoniae, betahaemolytic streptococcus of group A, Enterococcus faecalis and Staphylococcus aureus, including methicillin resistant S. aureus (MRSA) to erythromycin, azithromycin, other macrolides and lincosamides.
PHARMACOKINETICS:
Absorption
After oral administration the bioavailability of azithromycin is approximately 37%. Peak plasma levels are reached after 2-3 hours (Cmax after a single dose of 500 mg orally was approximate- ly 0.4 mg/l).
Distribution
Kinetic studies have shown markedly higher azithromycin levels in tissue than in plasma (up to 50 times the maximum observed concentration in plasma) indicating that the active substance is heavily tissue bound (steady state distribution volume of approximately 31 l/kg). Concentrations in target tissues such as lung, tonsil, and prostate exceed the MIC90 for likely pathogens after a single dose of 500 mg.
In experimental in vitro and in vivo studies azithromycin accumulates in the phagocytes, freeing is stimulated by active phagocytosis. In animal studies this process appeared to contribute to the accumulation of azithromycin in the tissue.
In serum the protein binding of azithromycin is variable and depending on the serum concentration varies from 50% in 0.05 mg/l to 12% in 0.5 mg/l.
Excretion
Plasma terminal elimination half-life closely reflects the tissue depletion half-life of 2 to 4 days. About 12% of an intravenously administered dose is excreted in the urine unchanged over a period of 3 days; the majority in the first 24 hours. Biliary excretion of azithromycin, predomi- nantly in unchangedform, is a major route of elimination.
The identified metabolites (formed by N-and O-demethylising, by hydroxylising of the desosamine and aglycone rings, and by the splitting of the cladinose conjugate) are microbio- logically inactive.
After a 5 day treatment slightly higher (29%) AUC values were seen in the elderly volunteers (>65 years of age) compared to the younger volunteers (< 45 years of age). However these differences are not regarded as clinically relevant; therefore a dose adjustment is not recommended